Endometriosis and the Immune System: The Hidden Connection
Endometriosis and the Immune System share a deeper connection than most people realize. Many women experience pain, inflammation, and hormonal changes, but the role of immunity often remains overlooked. This blog explains how Endometriosis and the Immune System influence each other, why this connection matters, and how understanding it can help patients seek the proper treatment at the right time.
What Is Endometriosis?
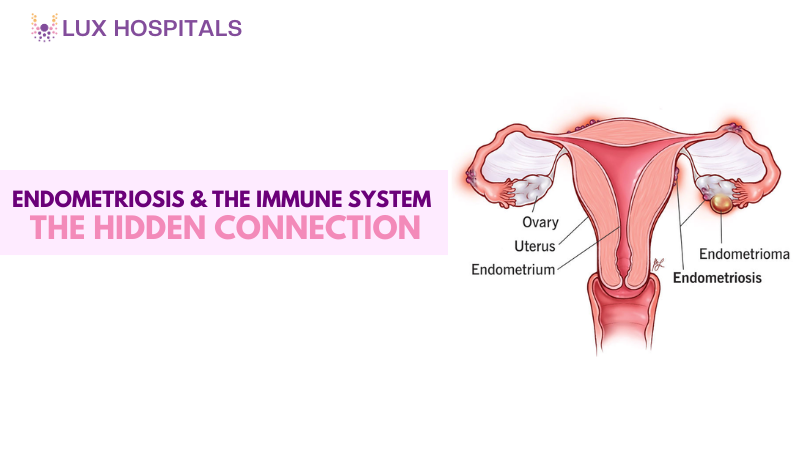
Endometriosis and the Immune System are linked because endometriosis itself is an inflammatory condition. When tissue resembling the uterine lining grows outside the uterus, it is known as endometriosis. The uterus. These tissues respond to hormones, causing:
- Severe cramping
- Chronic pelvic pain
- Pain during periods
- Painful intercourse
- Difficulty conceiving
As inflammation increases, the immune system responds—but sometimes in the wrong way.
How the Immune System Normally Works?
Before understanding the hidden connection between Endometriosis and the Immune System, it’s essential to know how immunity works.
The immune system protects the body by:
- Fighting infections
- Removing unwanted cells
- Preventing abnormal tissue growth
- Managing inflammation
A healthy immune response quickly identifies and destroys anything harmful. But in endometriosis, something changes.
How Endometriosis Affects the Immune System?
The relationship between Endometriosis and the Immune System begins when endometrial-like tissue implants outside the uterus. The immune system should recognize this tissue as abnormal and eliminate it, but in many women, this does not happen. Instead:
- Immune cells become less effective
- Inflammation remains high
- Damaged tissues are not repaired properly
- Pain worsens due to chronic inflammatory reactions
This weakened response allows endometriosis lesions to grow unchecked.
How the Immune System Contributes to Endometriosis?
Studies show that Endometriosis and the Immune System influence each other in both directions. When immunity is not functioning correctly, endometrial-like cells survive more easily outside the uterus.
Key Ways the Immune System Encourages Endometriosis
Decreased Natural Killer (NK) Cell Activity
- NK cells typically destroy abnormal tissue. In endometriosis, their activity is reduced.
Increased Pro-Inflammatory Cytokines
- These proteins worsen inflammation and pain.
Reduced Ability to Clear Retrograde Menstruation
- Many women experience menstrual blood flowing backwards into their pelvis. Still, endometriosis patients’ immune systems are unable to remove misplaced cells.
Overactive Macrophages
- These cells should remove debris, but instead they release chemicals that fuel inflammation.
This cycle increases pain and encourages lesion growth.
Symptoms Linked to Immune Dysfunction in Endometriosis
When Endometriosis and the Immune System are interconnected, symptoms become more severe.
Common immune-related symptoms include:
- Fatigue
- Chronic pelvic inflammation
- Lower immunity and frequent infections
- Severe period pain
- Digestive discomfort (bloating, IBS-like symptoms)
These signs show the impact of uncontrolled immune reactions.
Treatment Options Targeting the Immune System
When treating Endometriosis and the Immune System, modern medicine focuses on reducing inflammation, regulating the immune system, and relieving symptoms.
Effective Treatment Approaches
Hormonal Treatment
- Aids in reducing tissue growth and managing uncomfortable cycles.
- Anti-Inflammatory Drugs
- Reduce immunological activity and inflammation.
Immunomodulating Therapy
- Supports immune balance in women with severe inflammation.
Surgical Removal of Lesions
- Helps reduce pain and restores fertility in many cases.
Modifications to Lifestyle
- Anti-inflammatory diet
- Exercise
- Stress reduction
- Better sleep patterns
These methods help balance immunity naturally.
Conclusion
Understanding the relationship between endometriosis and the immune system is essential. Women can receive long-lasting relief and a more precise diagnosis by investigating both immunological and hormonal variables. To support women with endometriosis, hospitals such as Lux Hospitals prioritise patient-centred care and current medical recommendations. With greater awareness and improved treatment strategies, women can lead healthier, more comfortable lives.
Frequently Asked Questions
Endometriosis is impacted by the immune system's inability to eliminate aberrant endometrial-like cells that proliferate outside the uterus. Increased discomfort, inflammation, and tissue damage result from this feeble reaction. When immunity declines, endometriosis symptoms often worsen.
Yes, immune imbalances may contribute to endometriosis. When immune cells do not clear retrograde menstrual cells effectively, lesions can form. An overactive inflammatory response further supports the growth of endometriotic tissue.
Endometriosis can affect the immune system by causing chronic inflammation. Long-term pain and inflammation strain the immune system and may reduce overall immune efficiency. Some women with endometriosis experience fatigue and increased susceptibility to illness.
Endometriosis may be more common among women with autoimmune diseases, according to research. There is a substantial correlation between immune system dysfunctions and conditions like rheumatoid arthritis, lupus, and hypothyroidism.
Yes, treatments that control inflammation and regulate immunity can reduce symptoms. Anti-inflammatory diets, medicines, and stress reduction help improve overall immune function. Combining immune-focused treatments with hormonal therapy offers better long-term relief.























